Eye Health
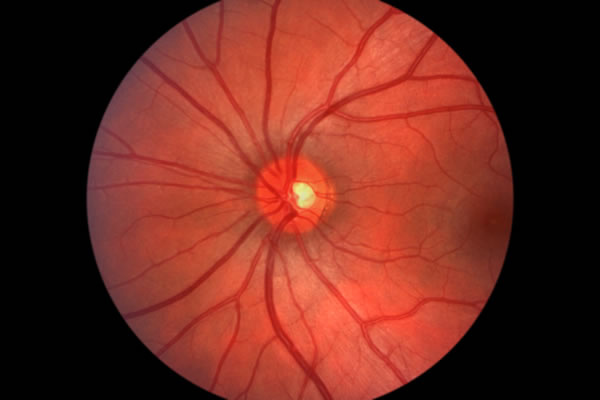
Most people experience eye problems at one time or another.
Visual problems may be minor or in some cases may require more specialised care.
Regular eye checks are important for the early detection of eye conditions and disorders.
Some of these common eye conditions are detailed below.
Someone who is myopic or short-sighted, will have difficulty seeing distant objects clearly. Myopia is very common and often begins to develop during teenage years, though many individuals become affected younger than this, or even in their later years. The exact causes for myopia are unknown. The current theory is a combination of genetics, excess near focusing, and more recently how objects are focused onto the peripheral retina. Myopia can easily be corrected with spectacles, or contact lenses, and if suitable with laser treatment.
Hyperopia, or "long-sightedness" is a condition which makes it difficult for people to see or focus comfortably at a close range. For some people reading up close can be blurred and glasses are generally required. For others, objects at close range may be clear, however more effort is required to see clearly, and hence their eyes get tired more quickly. These people experience difficulty concentrating when conducting tasks such as reading or when using the computer.
Like short sightedness or long sightedness, astigmatism is an optical condition of the eye which can affect the vision at close range, distance range or both. It is basically an irregularity in the shape of the cornea, where the front surface of the eye is more curved along one axis than the other. The ideal shape of a cornea is round like a soccer ball with the same curvature throughout. With astigmatism the front of the eye is shaped more oval like an Aussie rules football. Any difference in the curvature means that each axis of the cornea focuses light differently onto the retina and consequently the vision becomes defocussed. Astigmatism is most often combined with myopia or hyperopia. This condition can be corrected with spectacles, contact lenses or in some cases laser surgery.
Presbyopia is an age related progressive condition that makes it more difficult to focus objects at near. The first signs of this condition are often having difficulties focusing on print in phone directories, reading street maps or threading needles, even though distance vision may still be unaffected. Almost all people notice this problem creeping up on them after their 40th birthday, though some will be affected at an earlier age than this and some later (anywhere up to 50 years of age). Presbyopia is caused by a progressive loss of elasticity of the crystalline lens located inside the eye. This loss starts early in life but only creates difficulties in the middle age years. Currently mainly spectacles, and often contact lenses can correct the blurred vision that presbyopia causes. Surgery is also an option, however this will only correct the condition temporarily (several years) as it is a progressive disorder and eventually reading glasses will still be required.
Glaucoma is a condition in which nerve cells in the retina become damaged. These nerve cells are important in transmitting information about what we see to the brain. One of the risk factors for this condition is elevated pressure in the eye. Patients with advanced stages of this condition suffer from a loss in peripheral vision, or "tunnel vision" and ultimately may lose all of their vision. Unfortunately, damage to the nerve cells are not reversible. Usually there aren't any obvious visual symptoms that occur in the early stages of the disease, so this makes it very important for everyone, particularly for those aged over 40, or with a family history of glaucoma to have their eyes tested regularly.
Keratoconus is a condition that causes a thinning of the cornea, resulting in a protrusion at the front surface of the eye into a cone-like shape. As it progresses the vision becomes severely distorted, glasses don't work as effectively anymore, and the use of specially designed rigid gas permeable (RGP) contact lenses are needed. In the very advanced cases a corneal graft may be necessary to improve eyesight.
A cataract is a loss of transparency of the clear crystalline lens inside the eye. This can make it difficult to see clearly or to distinguish colours. Cataracts can grow uniformly throughout the lens, or only certain areas of the lens may be affected. Once present,cataracts are irreversible. Causes can be age, UV damage, trauma, certain medications, other ocular conditions or unknown factors. Treatment is usually via removal of the natural lens, and it's replaced by an artificial acrylic substitute (i.e. intra-ocular lens). This procedure is not a complicated one and has a very high success rate.
A pterygium is a degenerative condition of the conjunctiva that progresses across the conjunctiva and onto the cornea. It typically forms on the surface of the eye on the nasal side and has a triangular shape with the point towards the pupil. The tissue contains many blood vessels and as it grows in size it damages the superficial tissue of the cornea. Pterygia (plural) are usually harmless, though if allowed to grow large enough they can affect vision by changing the shape of the cornea or eventually by blocking the light entering the pupil. In these cases surgical removal is necessary.
About 250,000 older Australians have Age Related Macular Degeneration (ARMD). Some of these people have severely impaired vision and some are legally blind. ARMD affects the macula, which is the most important part of the retina responsible for central vision. When the health of the macula is affected, as in ARMD, vision can be dramatically affected.
People do not become blind with ARMD as they can still see to the sides, above and below the central vision. However in the centre, they develop a black or grey patch that prevents them from seeing clearly. Often the first sign for people with ARMD is that they see a distortion with straight lines, or that there is disturbance with their central area of vision.
There is no hard evidence as to why ARMD develops. Generally ARMD is not considered to be an inherited disorder. However, there is strong evidence that adequate amounts of vitamins and antioxidants are included in one's diet slows, and in some instances halts progress of the disease. Green leafy vegetables, coloured vegetables (e.g. Carrots, pumpkin, capsicums, tomatoes), and many variety of fish are rich in the appropriate antioxidants needed, and it is recommended that at least three servings per week are included in the diet.
Although there is no cure for ARMD, patients who have this condition should consult their optometrist to determine if there are any optical aids that can assist in reading or viewing the TV, and to provide advice on how to make best use of remaining vision.
Almost 1,000,000 Australians have diabetes. About half of these people are unaware that they have diabetes and many don't discover the disease until it affects them later on in life. For example, about 15% of diabetics already have evidence of diabetic eye disease at the time diabetes is diagnosed. Generally diabetic eye disease would indicate that the disease had been present for a number of years.
Diabetes affects the small blood vessels in the retina of the eye. The "walls" of the blood vessels weaken which will cause them to rupture, resulting in areas of haemorrhaging within the retina. If this is allowed to progress without any treatment, it can be very damaging to the health of the eye, consequently to their vision and eventually lead to blindness.
Usually when the eyesight is lost, it is irreversible. The tragedy of this is that in many instances these vision losses could have been avoided if detected early. Research has shown that tight control of blood sugar levels prevents or delays the onset of these retinal changes and subsequent retinopathy. "Tight control" usually means regularly checking of ones blood sugar levels, ensuring that it falls within the normal range.
With or without tight control, it is essential that those people with diagnosed diabetes have their retinas examined by an optometrist regularly. This is done during a simple in-office procedure (lasting about 30 to 40 minutes) with a dilated pupil. When viewing the retina, the optometrist via digital retinal imaging can look for and detect the presence of early retinal changes before any damage occurs, and if necessary can arrange an appropriate referral to a retinal ophthalmologist for any treatment, usually in the form of laser-type surgery.